How LED Phototherapy is Moving Into Recovery Focused Aesthetics
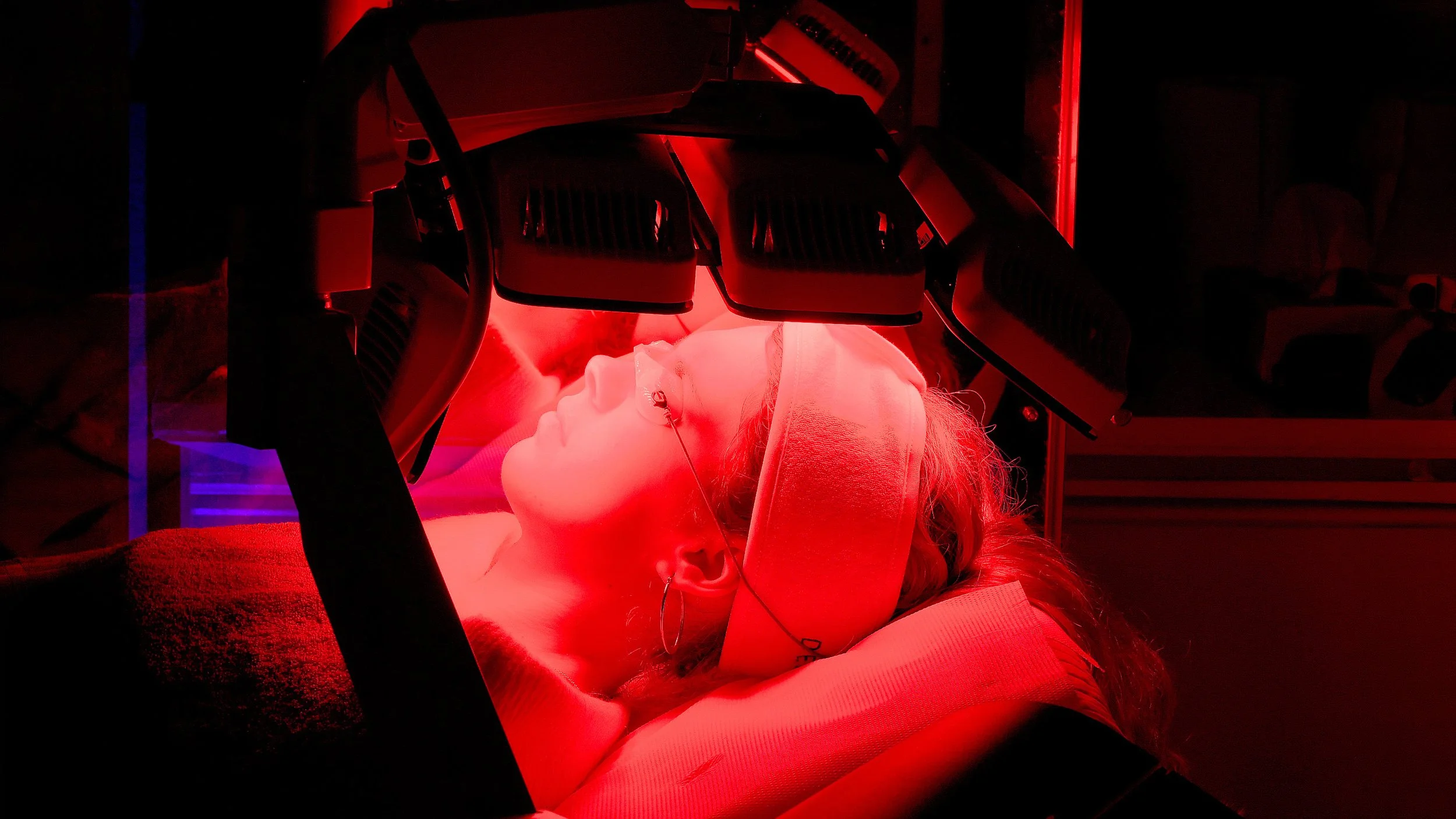
As advanced aesthetics places greater emphasis on recovery, clinicians are looking more closely at the technologies that can support tissue repair, regulate inflammation and improve patient comfort after treatment. LED phototherapy has long been used within acne and skin rejuvenation protocols, but its role is now widening. In clinic settings, it is increasingly being considered as part of a broader treatment plan that sits around a procedure, rather than as a standalone skin treatment.
Part of that shift comes from a stronger clinical focus on recovery itself. Post treatment care is no longer only about visible redness or the number of days a patient may need before returning to normal activity. It now includes questions around cellular energy, inflammatory control, tissue resilience and how well the body restores function after intervention. That has opened up more interest in modalities that can support those processes without adding further trauma.
This is where the power of phototherapy can come into play; red and near infrared light are used in relation to mitochondrial cytochrome c oxidase activity and ATP production, while also supporting microcirculation and inflammatory regulation. Blue light is positioned around antimicrobial activity and may also influence circadian rhythm and neurochemical pathways linked to alertness and mood. In practical terms, this places LED phototherapy within a wider discussion about how light based treatment may support recovery as well as skin quality.
That discussion is closely tied to mitochondrial health. Mitochondria are central to cellular energy production, and their efficiency is relevant to tissue repair, inflammatory balance and neuromuscular performance. Within both medical and aesthetic settings, there is increasing interest in how recovery may be improved by treatments that support lymphatic circulation, autonomic balance and photobiomodulation. LED phototherapy fits into that thinking because it can be introduced into treatment planning before or after a procedure without increasing invasiveness.
An unpublished observational protocol explored the use of Dermalux Tri Wave MD phototherapy alongside lymphatic drainage technology. Led by independent nurse prescriber and clinic director Kate Monteith Ross, INP and clinic director at The Clinic by La Ross, who designed the treatment protocol, and delivered in practice by senior massage therapist Courtney Vick, the four week protocol followed six medically well participants across 12 treatment sessions carried out three times per week. Three participants received lymphatic drainage technology alone, while three received lymphatic drainage technology combined with Dermalux Tri Wave MD phototherapy. Baseline and post treatment assessments included body composition measurements, physical measurements and self evaluation questionnaires covering energy, digestion, musculoskeletal comfort, mood, sleep quality, cognitive clarity and overall wellbeing.
According to the protocol, all participants showed measurable improvement across several outcome measures. Those receiving lymphatic drainage therapy alone reported reductions in abdominal discomfort, muscular tension and perceived bloating, together with better sleep quality and general wellbeing. Participants receiving the combined protocol were reported to show broader improvements across physical and psychological domains. These included greater reductions in joint discomfort and muscular tightness, improved digestive comfort, reduced perceived systemic bloating, and higher questionnaire scores relating to mood, sleep, cognitive clarity and perceived recovery.
The rationale for combining the two approaches is clinically straightforward. Lymphatic drainage technology is used to support lymphatic circulation, venous return and interstitial fluid movement. These functions matter because the lymphatic system contributes to immune modulation, metabolic waste clearance and tissue homeostasis. Reduced lymphatic flow has been associated with tissue congestion, chronic inflammation and reduced cellular efficiency. Pressure based lymphatic stimulation may also support parasympathetic nervous system activation, which has relevance for digestion, sleep quality and stress response. When that is combined with photobiomodulation, the aim is to support recovery at both a systemic and cellular level.
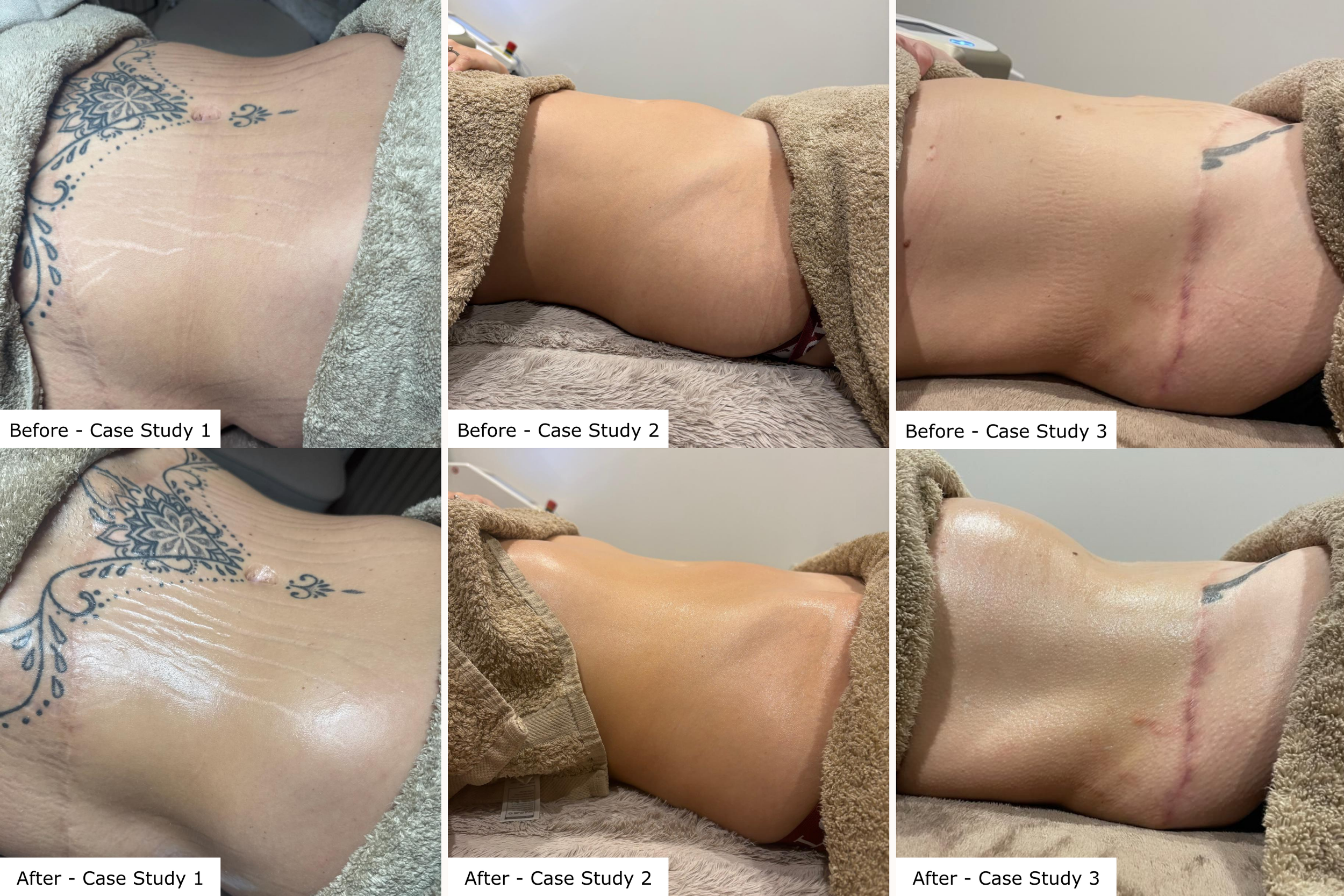
The before and after case study imagery show views from three cases following one treatment of manual lymphatic drainage and a 20 minute session of red and near infrared Dermalux Tri Wave. The photographs suggest short term visible changes in contour and tissue appearance,
Monteith Ross said: “This preliminary clinical work suggests that combining lymphatic drainage technology with Dermalux Tri-Wave MD phototherapy may enhance outcomes compared with pressure therapy alone. The improvements observed across physical comfort, sleep, mood and cognitive clarity may reflect the combined effects on lymphatic function, autonomic regulation and mitochondrial activity. While larger controlled studies are needed, the findings support further exploration of combination treatment pathways within recovery focused clinical practice.”
This observation, if proved in a wider setting, could encourage LED phototherapy to be discussed less as a simple add on and more as a support tool within a wider care pathway.
Recovery support is becoming a more defined part of treatment planning, and technologies that fit into existing workflows without requiring additional downtime are likely to remain of interest. LED phototherapy appears well placed within that shift, particularly in pre treatment preparation, post procedure support and longer term skin health planning. The next stage for the category will depend on stronger published evidence and a clearer understanding of where these protocols deliver the most value in everyday practice.